Virtual Patient Visits: The Role of Technology in Adjusting Practice Patterns
Having confidence that patients can be safely and effectively monitored and followed remotely is a significant factor in delivering high-quality care
W hile much has changed with respect to medical encounters due to the COVID-19 pandemic, delivering excellent patient care remains the top priority. That means that while the format of the patient encounter may be different, patients expect—and frankly deserve— no drop off in terms of the quality of that encounter.
In our clinic, we were not using any telemedicine prior to the pandemic. Now, it has become a useful tool for reserving our in-person visits for patients requiring procedures or face-to-face time with the doctor. After briefly halting non-emergency services early in the pandemic, our clinic is back to nearly full volume and workflow. In order to minimize patients’ time in the practice, testing and imaging is performed as usual, but it is reviewed after they leave. We then conduct a virtual consultation to go over the findings and discuss future care plans; if needed, patients are called back for additional in-person follow-up.
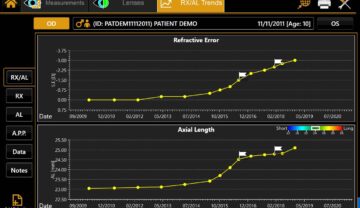
Frankly, one important reason we are able to accommodate working conditions that are more reliant on virtual interactions is because of the quality of the imaging platforms we have at our disposal. We are probably performing even more imaging on our patients with age-related macular degeneration and diabetic eye diseases than we were prior to the pandemic. It is easy to appreciate that these conditions are time sensitive, meaning that avoiding vision loss depends on recognizing changes in anatomy in a timely fashion and implementing treatment accordingly. The use of widefield imaging and the multimodal, swept source DRI OCT Triton (Topcon Healthcare, Tokyo, Japan), which combines swept source OCT technology and non-mydriatic fundus photography on one platform, gives us confidence that patients are being examined thoroughly, thereby allowing us to limit visits.
The role of technology in patients’ safety
Overall, technology has always been an important part of our practice, but it has become even more integral during the pandemic. The ability to closely monitor and follow patients with the confidence that crucial pathology will not be missed, as noted above, is one way we have come to rely on technology. Another example of technology that we implemented during these changing times is an artificial intelligence facial recognition software (AI Fever Check; Horizons) used to noninvasively measure patients’ temperature upon arrival. Initially we started out with a staff member outside the office checking temperatures and asking questions; this new system obviates the need to dedicate a staff member to this task. On the one hand, this exemplifies how technology can serve to improve efficiency, but more cogently, it also shows how it can contribute to safer working conditions, as we are limiting direct contact with patients with unknown viral status.
In some respects, the pandemic has altered perceptions on the benefits of technology in our daily lives. Ordering online has become commonplace, and consumers are using their phones and computers to communicate while maintaining social distance. The idea that we can all still experience life because of technology, yet do so more safely because we are virtual, is something that is likely to reshape our world going forward. As medical providers, we would be overlooking the obvious if we think that mindset will not affect patients’ expectations for the medical encounter. Indeed, we get the sense that patients have increased confidence coming into the clinic because we have adopted technology that contributes to greater safety. For example, we use an ultraviolet light to decontaminate hard surfaces after patient visits. Its use is backed by strong scientific rationale, and yet equally as important is the fact that using this simple device communicates to patients that we are concerned for their safety, that we have their best interests in mind, and that we are taking active steps to protect their health.
Lessons for the future
There is no question that maintaining standards of care while practicing virtual medicine places additional stress on the medical team. There has been little, if any, pushback from patients in terms of the changes we have had to make because of the pandemic, including reduced in-office time, limited interactions with staff and physicians, and the need to wait outside the building until appointment time. That is to say, patients are largely doing their part to adjust, and so the onus is really on the care team to make patients feel safe. That is not necessarily a foreign concept to eye care, a specialty that has always been attuned to patients’ experiences. In these anxious times, the need to maintain that focus is doubly important, because anything we can do to help patients feel safe and confident in their health care facility is more than likely going to be worth the effort. And that should be a lesson we take with us as we move forward and think of a world beyond the pandemic.
What we have learned about technology during the pandemic and what it can contribute to our patients’ experience in the clinic is likely to inform a new model for practice. For instance, we have learned that virtual care is simply more convenient for a wide array of patients and does not have to contribute to a loss of volume. In fact, it may help expand a provider’s ability to care for more patients. For some individuals, such as those with mobility issues or difficulties traveling to the clinic, having the ability to use virtual medicine might significantly improve access to eye care services. Where these kinds of services fit in the schedule and how best to integrate them will be based on the practice’s location, patient base, and other factors, but overall, having dedicated time to see patients virtually is a benefit, it is safe, and it is convenient for all parties.
Most importantly, because of how eye care technology has advanced, providers can have confidence that quality of care will not be compromised by going virtual. Devices like the DRI OCT Triton consistently and reliably deliver images that help to identify early-stage pathology and subtle architectural changes when implementing treatment is meaningful for the long-term outcome. Integrating these kinds of devices into virtual practice protocols has a very real chance of improving patients’ safety now while expanding access to services, and thereby enhancing care delivery, during the next new normal.

ABOUT THE AUTHOR
NETAN CHOUDHRY, MD, FRCSC(C), DABO is the Medical Director, Vitreous Retina Macula Specialists of Toronto. Financial disclousures include: Consultant (Novartis, Roche); Consultant and Speaker (Allergan); Speaker and Advisor (Bayer, Optos, Topcon); Researcher (ZEISS)